Is the ultrasound scan safe for your baby? What is a 3D scan?
An ultrasound scan is an assessment tool commonly used by doctors during your pregnancy. It is a safe and useful way of obtaining images of your baby and his/her surrounding environment to provide useful information on his/her health (Figure 14.1).
Dating Scan (Week 6–12)
Your first ultrasound scan should be performed in your first trimester of pregnancy. In a usual situation, the scan will show the early pregnancy sac in the womb with the fetus within the sac. This can be seen as early as 5 to 6 weeks of pregnancy. Visualising the pregnancy in the womb is reassuring, because it confirms that it is in the right location.
Although very uncommon, pregnancy can sometimes be implanted in the wrong place like in the fallopian tubes (known as
ectopic pregnancy). This happens to 1– 2% of all pregnancies.
The baby’s heartbeat is normally visible by 6 weeks of pregnancy. Sometimes, your doctor may use a vaginal probe for the scan when your pregnancy is about 5 to 6 weeks. Be assured that vaginal scanning is safe and will not harm your pregnancy in any way.
The current gestation (age) of your pregnancy can be calculated by taking measurements of your baby during the scan (Table 14.1).
Your expected date of delivery (EDD) can then be estimated accurately. This is especially important for your doctor to manage your pregnancy well.
It also helps you to plan ahead like informing your employer about maternity leave and making all the necessary arrangements for baby care before the arrival of your baby.
Indeed, the accuracy of the first trimester ultrasound scan is within a week. The first trimester ultrasound also allows you to know if you are expecting twins or even triplets.
Nuchal Translucency Scan (Week 11–14)
In recent years, ultrasound scans in the first trimester can be used to assess the risk of your baby being affected by Down Syndrome (read the article on Down Syndrome Tests).
This is done by a measurement of the skin fold thickness (nuchal translucency) at the back of the baby's neck. If the neck fold is unusually thick, it may indicate that your baby may have Down syndrome.
Other causes may include heart abnormalities or even other rarer genetic syndromes. This test is quite accurate to detect Down Syndrome as the detection rate is 80% in the hands of experienced doctors. So do consider this test, which is perfectly safe for your baby.
If your baby is in an optimal position, ultrasound examination after 11 weeks may be able to visualize the baby’s nose bone (known as nasal bone). The absence of the nose bone is a worrying sign, which increases the risk of Down Syndrome.
Screening Scan (Week 18–22)
Being an expectant mother, you will find it reassuring to know that your baby will be born healthy with no congenital deformities. An ultrasound scan can be used for screening to look for abnormalities in the physical structure of the baby, for example in the heart, lungs, spine, brain, long bones in legs or arms, organs in the abdomen like liver, stomach, intestines, kidneys, bladder and even check for cleft lip and palate.
Finding of certain abnormalities during an ultrasound scan may also alert doctors to the possibility of Down Syndrome or other genetic abnormalities in the baby. Further testing can then be done to exclude these.
Ultrasound screening for physical abnormalities is usually done during around the fifth month or 20th week of your pregnancy. It is performed by a sonographer or obstetrician, using a fairly advanced ultrasound machine that provides excellent resolution for imaging. The accuracy of scans is about 70% in detecting all abnormalities.
Note:
Although a structural screening scan is undertaken, detection of structural problems will never be 100% accurate. Detection rates may vary and be reduced by factors such as
maternal obesity, abdominal scars, fetal position and reduced amniotic fluid.
Growth Scan (32–36 weeks)
Later in pregnancy, it is important to monitor your baby’s growth. Your doctor will monitor this, most of the time by examining you and measuring the height of your tummy during your regular visits.
Ultrasound scan from late second trimester may help to confirm that your baby is growing well. We can also tell if the amniotic fluid in the “water-bag” is sufficient for the baby. This tells us about the health status of baby.
This scan is also useful to determine your baby’s position and the placenta location in the womb. This will help your doctor decide if it would be safe to deliver your baby through the normal birth passage, or if a Cesarean section may be necessary.
Doppler Scan
Sometimes, a more specialised mode of ultrasound called a Doppler ultrasound scan may be used for more specific conditions.
For example, when the growth of the baby is reduced or anemia (low hemoglobin) is suspected in the baby. Doppler scan can help to provide additional information on the blood flow status of the placenta and the health status of the baby.
Did You Know?
-
You may be able to determine your baby's sex with an ultrasound scan after 16-20 weeks after gestation.
-
All your baby's organs are formed by 16 weeks gestation.
-
At 16 weeks gestation, your baby weighs around 146g and is about 12cm long, about the size of an avocado.
-
Your baby can now hear your voice and heartbeat. Music and mother's voice are calming to the baby.
-
Your baby can also make sucking, swallowing and breathing movements.
-
Your baby's heart is now pumping about 6 gallons of blood a day!
Frequently Asked Questions
1. What do I expect at an ultrasound scan?
You will be asked to lie on a couch, back down. The lights will be dimmed so that it is easier for the doctor to see the images of your baby. An ultrasound scan is done with placing the scan probe on your tummy. Before that some gel will be applied on your tummy. In the early weeks of pregnancy, a probe placed through the vagina may be used to see your baby clearly.
2. When should I go for my first ultrasound scan in pregnancy?
Having a scan during the first trimester (first 12 weeks) is very useful for you to know your gestation and due date. This is important for your doctor for optimal management of your pregnancy. However, having a scan too early in pregnancy will not yield the necessary information, as the developing baby is not seen on scan until 5–6 weeks of pregnancy (from the first day of your last menses if you have a regular 28-day cycles). Measurements of the baby can be done more accurately after 8 weeks gestation. The most ideal time for dating scan is between 8 to 12 weeks of pregnancy.
3. Is an ultrasound scan safe for my baby?
While the safety of ultrasound scans in pregnancy is endorsed by professional experts and is now a common tool in pregnancy assessment, it is still important to exercise prudency. You should understand the purpose and reason for each ultrasound scan. Also, doctors would ensure that each ultrasound examination is done carefully within a reasonable time.
4. What is a 3D scan and do I need one?
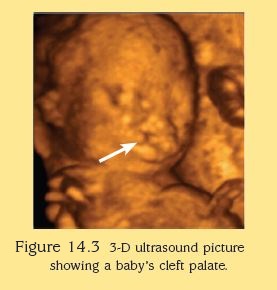
A 3D ultrasound can furnish us with a three-dimensional image of the fetus. The transducer takes a series of images and the computer processes these images and presents them as a three-dimensional image. These costly scans are regarded as “social scans” at the present moment and generally do not add value to the diagnosis of fetal structural problems. Occasionally, it can help to delineate small structural problems such as abnormality in the fingers or toes and minor skin defects. Most hospitals do not offer 3D scans as a routine scan.
5. What is the chance of my baby having a major fetal abnormality?
The risk in the general population that a fetus has a major structural birth defect is 2–3%. While not all abnormalities can be identified by ultrasound scans, many can be. When a comprehensive examination of the fetus is normal, the risk of a major abnormality is about 1%. Some structural problems like heart defects may recur in subsequent pregnancies. Do consult your doctor who will counsel you on the risks accordingly.
Acknowledgement
Source: Dr TAN Thiam Chye, Dr TAN Kim Teng, Dr TAN Heng Hao, Dr TEE Chee Seng John, The New Art and Science of Pregnancy and Childbirth, World Scientific 2008.
Visit Parent Hub, for more useful tips and guides for a healthy pregnancy.
Download the HealthHub app on Google Play or Apple Store to access more health and wellness advice at your fingertips.

HealthHub AI

























